Due to a recent change in our pharmacy software system, the process for submitting refill requests online has now changed.
Our previous mobile app and your current login credentials will no longer work.
Please click the Patient Portal tab to begin the new process.
Thank you for your patience during this transition.
Get Healthy!
- Dennis Thompson
- Posted December 1, 2023
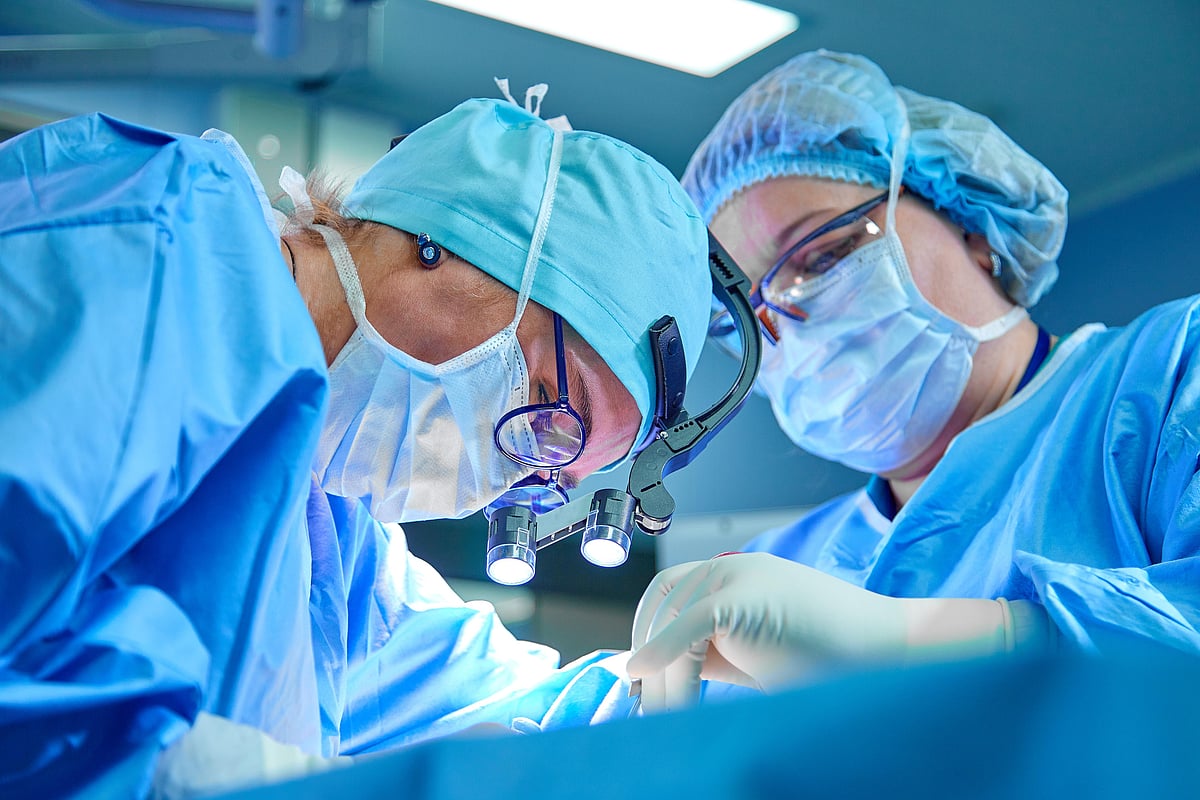
Treatment Used on Donated Hearts May Be Useless, Even Harmful: Study
A technique doctors use to preserve donated organs is actually doing no good, and might even be harming the organs, a new study reports.
Physicians routinely dose deceased organ donors with thyroid hormones, in a bid to preserve heart function and keep the donors' organs healthy and viable.
But thyroid hormone treatment made no significant difference in the number of hearts successfully transplanted from a group of more than 800 organ donors, according to results published in the Nov. 30 issue of the New England Journal of Medicine.
Further, thyroid hormone was more likely to cause high blood pressure and increased heart rate in the bodies of deceased donors, researchers found.
"We found good evidence that this intervention we've been using for 40 years doesn't work,"said researcher Dr. Raj Dhar, a professor of neurology at Washington University in St. Louis. "Our findings tell us we should halt this practice."
Managing deceased donor bodies by administering thyroid hormone is a procedure that's been adopted by more than 70% of organ-procurement organizations and is used on thousands of organ donors each year, researchers said.
But no one has ever rigorously studied whether giving the hormone to donors on life support actually improves the success rate for donations, he said.
Donor patients declared brain dead can provide up to eight organs, if all are in good shape, but it can take up to 72 hours from the time of brain death for a transplant surgery to take place.
During that time, doctors work to keep donors' hearts beating as normally as possible, to preserve the health of the organs.
Despite those efforts, about half of all such hearts deteriorate and are not suitable for transplantation when the time comes, researchers said.
"It's vital that we explore questions like this to ensure we are doing all we can for patients who need organs -- and to ensure that they receive the most benefit possible from the generous people who choose to donate organs,"Dhar said in a university news release.
Previous observational studies had suggested that thyroid hormones might increase the viability of a still-beating donor heart. Thyroid hormones influence heartbeat, and levels of the hormone can decline once the brain stops working.
However, some doctors have been concerned that providing IV thyroid hormones to a donor body might increase the risk of fast heart rate and high blood pressure -- potentially damaging the heart and other organs.
For this study, a team across 15 organ-procurement organizations nationwide randomly assigned half of a group of 838 deceased organ donors to receive a synthetic thyroid hormone called levothyroxine. The rest were just given a saline drip.
Just over half of the hearts from each group were suitable for transplantation -- 230 (55%) from the thyroid hormone group and 223 (53%) from the saline placebo group.
Of those, about 97% of the thyroid-treated hearts and 96% of the placebo-treated hearts still worked well for recipients after 30 days.
But doctors also found that high blood pressure and fast heart rate in deceased donors' bodies became less severe or disappeared when thyroid hormone doses were reduced or discontinued, suggesting that thyroid might be causing overstimulation of the hearts.
"It turns out that it doesn't have any benefit and may cause some harm,"Dhar said.
After seeing the trial results, several organ-procurement organizations have stopped using thyroid hormone in treatment of organ donors, Dhar noted.
More information
The Mayo Clinic has more about organ donation.
SOURCE: Washington University, news release, Nov. 29, 2023
